The following guidelines are based largely on the work of Neal Benowitz, et.al. These numbers were derived from serum cotinine values as measured by HPLC/MS. Note that optimal cut‐points differ by race/ethnicity and sex. We encourage you to read the entire text of the 2009 article. (1)
| Race/Ethnicity | Adult Cutoff | Adolescent Cutoff |
|---|---|---|
| Non‐Hispanic whites | 5 ng/mL | 3 ng/mL |
| Non‐Hispanic blacks | 6 ng/mL | 3 ng/mL |
| Mexican-Americans | 1 ng/mL | 1 ng/mL |
| Gender | USA Cutoff |
| Adult Male | 1.78 ng/mL |
| Adult Female | 4.47 ng/mL |
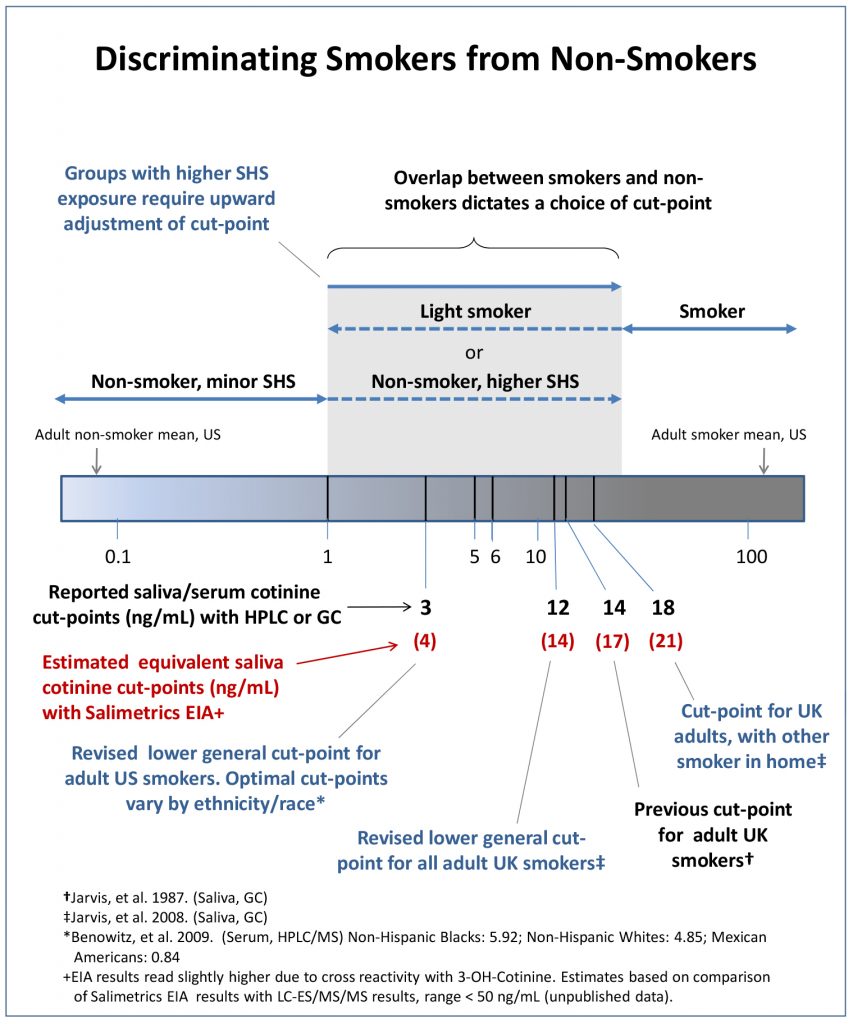
Note: Saliva cotinine values are slightly higher than in serum by a ratio of 1.16. (2) In addition, EIA results give values higher than HPLC or CG methods due to cross ‐reactivity with 3‐OH‐cotinine, a metabolite of cotinine.
When using the Salimetrics Cotinine EIA cut points should be adjusted accordingly. (See figure on p. 2.)
For additional discussion of cut‐points and a comparison with UK levels see articles by Jarvis, et al. (3,4)
 Contact: Salimetrics (USA)
Contact: Salimetrics (USA)