Drop Date: October 2021
DHEA & DHEA(S) – The Stress Whisperers
In This Drop: DHEA & DHEA(S) – The Stress Whisperers
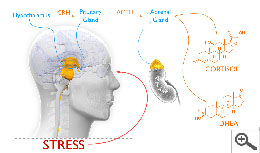
DHEA and cortisol are both hormones produced by the adrenal glands. While DHEA and cortisol are often measured independently as biomarkers, measuring the two hormones together can offer advanced insights for continued stress research.
As salivary cortisol becomes more widespread, researchers can increase innovation and have a better picture of behavioral problems by assessing multiple salivary analytes (Chen 2015). Assessing DHEA/DHEA(S) together with cortisol exemplifies this advantage. Strong evidence suggests that DHEA and DHEA(S) influence stress and behavior through anti-glucocorticoid effects. Early observations of this include below normal DHEA(S) levels observed in patients with Cushing’s syndrome. However, blocking glucocorticoid production results in an increase in DHEA levels (Kalimi 1994).
Although the underlying mechanism is still unclear, DHEA is believed to indirectly regulate glucocorticoid activation. DHEA indirectly increases levels of type 2 11β-HSD, causing greater conversion of glucocorticoids to the inactive state and decreasing overall glucocorticoid activity (Balazs 2008). Thus, the anti-glucocorticoid effects of DHEA indicate that there is an indirect relationship between cortisol and DHEA. This is illustrated by numerous studies of behavioral disorders that have found the ratio of cortisol to DHEA to be a useful predictor of symptoms and identifier of risk.
The DHEA and cortisol relationship is also useful when studying behavioral disorders, like depression and PTSD. A study focusing on attachment behaviors in adolescents found that fear of separation predicts higher waking cortisol/DHEA ratios as well (Oskis 2015). It is suggested that the high cortisol levels associated with anxious attachment styles result in a shift towards glucocorticoid synthesis, which, without buffering from DHEA, causes increased vulnerability to negative psychological outcomes. High cortisol levels can also impact other compounds leading to a reduction in immune and inflammatory response as well as cognitive dysfunction (Chen 2015).
PTSD has been previously linked to high DHEA levels, but a study of veterans with and without the disorder revealed that this relationship also involves cortisol. High DHEA levels relative to cortisol are indicative of greater adversity experienced and risk factors for PTSD. High DHEA levels alone suggest increased severity of PTSD symptoms (Yehuda 2006). A study of PTSD in women supported these findings. Women with PTSD show higher DHEA/cortisol ratios compared to those without, and furthermore, those with both PTSD and depression display lower ratios than women with PTSD but not depression (Gill 2008).
Salivary DHEA(S) also shows a diurnal rhythm and awakening response that may help pinpoint distinct biological conditions in opposition of salivary cortisol. The cortisol to DHEA(S) ratio, for example, is also considered a ratio of catabolic to anabolic activity and can be useful for predicting HPA axis dysfunction (Guilliams 2015). While DHEA and DHEA(S) are both promising biomarkers for continued research and development, DHEA(S) exists at much higher levels and is considered a more stable biomarker for measuring stress-related conditions.
Both the cortisol to DHEA(S) ratio and cortisol to DHEA ratio have been a growing trend in clinical research to better understand the significance of measuring these two biomarkers together. When studying either cortisol or DHEA/DHEA(S), it’s a good idea to take the other into consideration as well as to account for any interactions between these prominent salivary analytes.
REFERENCES & RELATED RESEARCH
- Kalimi, Mohammed, et al. (1994). “Anti-glucocorticoid effects of dehydroepiandrosterone (DHEA).” Molecular and Cellular Biochemistry. 131.2:99-104.
- Balazs, Zoltan, et al. (2008). “DHEA induces 11β-HSD2 by acting on CCAAT/enhancer-binding proteins.” Journal of the American Society of Nephrology. 19.1:92-101.
- Kimonis, ER., et al. (2019). “Dehydroepiandrosterone (DHEA) and its ratio to cortisol moderate associations between maltreatment and psychopathology in male juvenile offenders.” Psychoneuroendocrinology 101:263 – 271.
- Goodyer, I. M., J. Herbert, and A. Tamplin. (2003). “Psychoendocrine antecedents of persistent first-episode major depression in adolescents: a community-based longitudinal enquiry.” Psychological Medicine. 33.460:1-610.
- Oskis, Andrea, et al. (2015). “Biological stress regulation in female adolescents: a key role for confiding.” Journal of Youth and Adolescence. 44.5:1066-1077.
- Chen, F.R., et al. (2015). “Tactics for modeling multiple salivary analyte data in relation to behavior problems: Additive, ratio, and interaction effects.” Psychoneuroendocrinology. 51:188-200.
- Gill, Jessica, Meena Vythilingam, and Gayle G. Page. (2008). “Low cortisol, high DHEA, and high levels of stimulated TNF‐α, and IL‐6 in women with PTSD.” Journal of Traumatic Stress. 21.6:530-539.
- Guilliams, Thomas G. “The Role of Stress and the HPA Axis in Chronic Disease Management.” N.p.: Point Institute, 2015. Print.
- Orta, OR,. Et al. (2020). “The association between abuse history in childhood and salivary rhythms of coristiol and DHEA in postmenopausal women.” Psychoneuroendocrinology. 112:104515
- Yehuda, R., et al. (2006). “Clinical correlates of DHEA associated with post‐traumatic stress disorder.” Acta Psychiatrica Scandinavica. 114.3:187-193.
- Granger, D., Kivlighan, K. ( 2003). “Integrating biological, behavioral, and social levels of analysis in early child development.” Child Development. 74(4): 1058-63.
*Note: Salimetrics provides this information for research use only (RUO). Information is not provided to promote off-label use of medical devices. Please consult the full-text article.
 Contact: Salimetrics (USA)
Contact: Salimetrics (USA)